The NHS Ceiling Is Falling In
In 2023–24, £900 million meant for NHS repairs was moved to cover day-to-day costs. The maintenance backlog is now £15.9 billion. The NAO says £49 billion. Seven NHS hospitals are being held up by metal props. Five won't start construction until 2037. The ceiling doesn't read the budget.
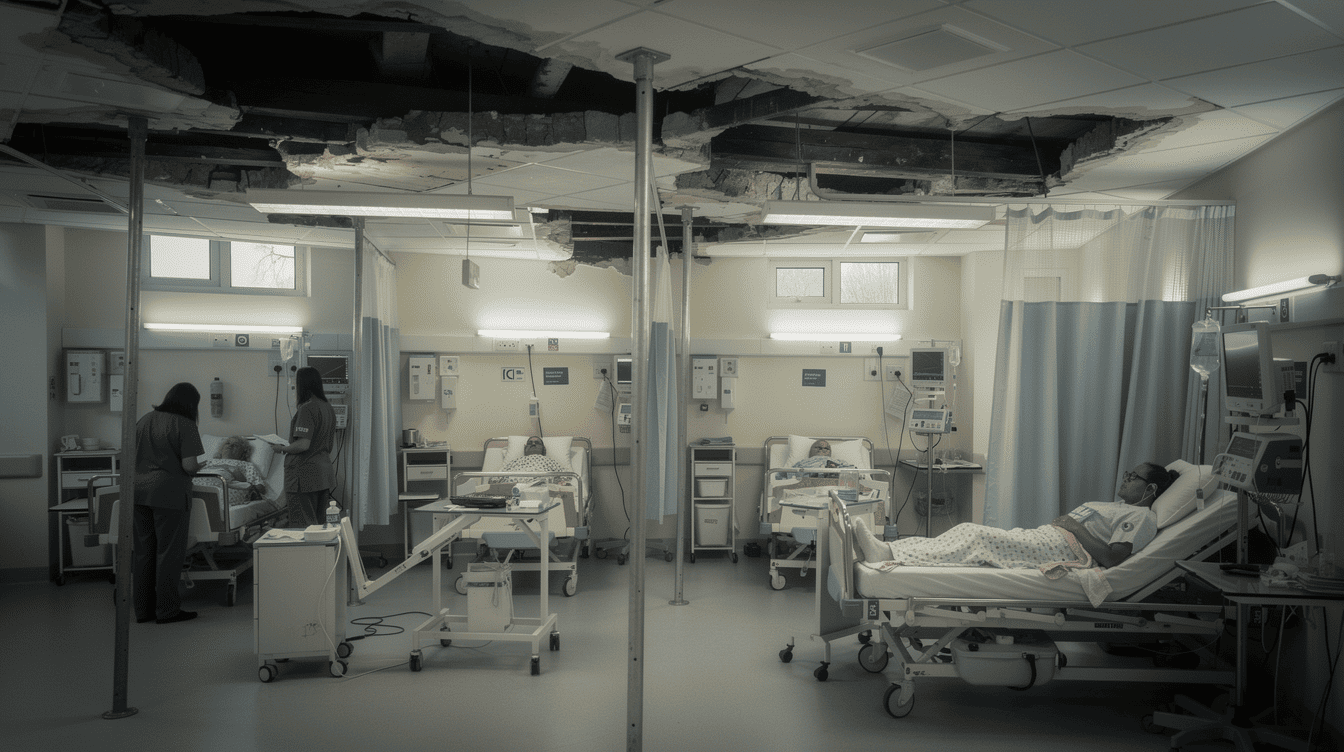
You won't have heard of it, but Reinforced Autoclaved Aerated Concrete was the material of choice for British public construction from the mid-1950s through to the 1990s. Cheaper than standard concrete, lighter, aerated with air bubbles, it was used in flat roofs, walls, and floors across schools, courts, and hospitals. Its designed lifespan was approximately thirty years. Many of the hospitals built with it are now fifty years old.
When RAAC is exposed to moisture, water penetrates the bubbles, reaches the steel reinforcement, and corrodes it from the inside. The material degrades not gradually but suddenly. The first visible sign is often the last warning.
Seven NHS hospitals have been confirmed as requiring full rebuilds:
- Queen Elizabeth Hospital in King's Lynn
- West Suffolk Hospital
- James Paget University Hospital
- Airedale General
- Frimley Park
- Hinchingbrooke, and
- Leighton Hospital in Cheshire.
Leighton is 60% RAAC and fifty years old, twenty years past its designed lifespan. Over £113 million has been spent since 2020 on inspection and remedial works. The repairs can stabilise the structure. They cannot reverse the damage.
At King's Lynn, the trust spent three years building a steel support structure to hold up the roof. In plain terms: the hospital is being kept open by scaffolding. As of September 2025, 41 hospital sites in England have confirmed RAAC (and as many schools). Twenty have eradicated it. Eighteen of the forty schemes announced under the New Hospital Programme, originally due to open in 2030, will not begin construction until 2030. Five may not start until 2037 to 2039. The buildings in the meantime remain open, staffed, and treating patients.
Construction experts have warned that if rebuilding is not accelerated, some hospitals may have to close before their replacements are ready. The Institution of Structural Engineers recommends no-walk zones on RAAC roofs, restrictions on removing or adding equipment, and humidity controls. These are not the conditions under which twenty-first-century medicine is delivered.
£15.9 Billion, and the Number Is Growing
The RAAC hospitals are the visible part. The total estimated cost to clear the NHS maintenance backlog reached £15.9 billion in 2024–25, up 15.7% on the previous year and more than 72% higher than the £9.2 billion estimated five years earlier.
This is not planned maintenance. It is the cost of work that should already have taken place: repairs the NHS owed its own buildings and did not pay. The sum now exceeds the £14 billion annual cost of running the entire NHS estate. The maintenance debt is larger than the operating budget of the infrastructure it covers.
The fastest growth is in the highest-risk category. Repairs classified as urgent to prevent catastrophic failure or disruption to clinical services now total £3.5 billion, up 28% in a single year. Significant-risk repairs add a further £5.6 billion. Together, nearly £9 billion of work the NHS knows it must do and cannot fund.
None of this is disputed. These are figures from the NHS's own Estates Returns Information Collection, signed off annually by chief executives.
The Capital Budget as Cashpoint
The mechanism is familiar from every preceding piece in this series, applied here to concrete instead of council accounts.
In 2023–24 alone, £900 million of capital funds for buildings and equipment was redirected to cover day-to-day running costs, while the maintenance backlog stood at £13.8 billion. Between 2014–15 and 2018–19, the Department of Health and Social Care transferred £4.3 billion from the capital budget into revenue. The pattern held for a decade: when the revenue budget ran short, capital was raided. When capital was raided, repairs were deferred. When repairs were deferred, the backlog grew.
In December 2024, the Treasury banned this practice. The rule was not preventative. It was a belated admission something had been happening for years which should never have been permitted. The damage was already baked into every wall and roof it sought to protect.
Lord Darzi's independent investigation, published in 2024, identified a £37 billion shortfall in capital investment relative to comparable countries during the 2010s. Forty new hospitals were promised. None have been built.
When the Roof Leaks, the Ward Closes
Infrastructure failure in the NHS produces approximately 5,400 incidents per year affecting service delivery: cancelled operations, ward closures, equipment failures, water leaks, electrical faults caused directly by the state of the buildings. This data needs to be verified against ERIC but appears accurate.
Modern medicine is infrastructure-intensive in ways that admit no flexibility. An MRI scanner requires stable power and controlled temperature. A sterile theatre requires intact walls, functioning ventilation, and consistent humidity. An intensive care unit requires every system to work continuously. The building is not peripheral to the healthcare. It is part of it.
The NHS estimates around 30% of the 2.4 million patient safety incidents reported each year result in some degree of harm, with approximately 12,000 leading to severe harm or death. A Public Accounts Committee report in early 2026 found a system overwhelmed by safety recommendations it cannot action. Total accumulated clinical negligence liabilities in England now stand at £60 billion.
Hiring Freezes in a Staffing Crisis
While the estate crumbles, the NHS is simultaneously preventing qualified staff from working in it.
Nursing applications in England fell to a record low in February 2025: 23,730, down 35% from 36,410 in 2021. The pipeline is contracting. At the same time, trusts under financial pressure have imposed recruitment freezes across the country. The NHS has over 43,000 nursing vacancies. Newly qualified nurses cannot fill them.
One nursing graduate, shortlisted for a national award for her work in end-of-life care, applied for 35 NHS jobs without success. She moved back to Nottingham and took a job in a coffee shop. At one trust, a graduating cohort of 20 nurses found two available posts. At another, there was one.
The trusts are not hiding vacancies they could fill. They are suppressing vacancies to protect revenue targets. The same trade-off applied to capital budgets, now applied to people. Providers were on course to spend £8.3 billion on temporary staffing in 2024–25. The agency bill exceeds what permanent hires would have cost. The trust pays it, records an overspend on temporary staff, freezes another permanent post to compensate, and repeats.
District nursing has contracted 47% since 2009. As community capacity has declined, patients have shifted into acute hospitals. Acute hospitals are overcrowded. Ambulances queue outside A&E for hours. The Royal College of Emergency Medicine estimates these delays cause 14,000 excess deaths every year. That is more than double all British armed forces' combat deaths since 1948.
The Ceiling Does Not Read the Budget
Revenue targets are set. Capital is raided to meet them. Repairs are deferred. The backlog grows. Staff are frozen out to protect the balance sheet. Agency workers fill the gaps at higher cost. The cycle restarts.
The building does not participate in this process. The concrete absorbs moisture at the rate determined by its composition and age. The steel corrodes at the rate determined by chemistry. The structure weakens at the rate determined by physics. The chief executive of NHS Providers put it plainly: critical parts of the NHS are falling to bits, literally, after years of underinvestment.
Clap for carers.
Our NHS.
Free at the point of delivery.
Seven hospitals are held up by metal props. Their replacements were promised by 2030. Eighteen of those schemes will not break ground until 2030. Five will not start for another decade after that.
The ceiling either holds or it does not.
- What was promised: World-class hospital infrastructure, modernised through record investment and a programme of forty new hospitals
- What exists: A £15.9 billion maintenance backlog growing at 15.7% annually, seven hospitals requiring structural props to remain open, and replacement schemes deferred to 2037
- What happens when they meet: Patients are treated in degrading buildings, operations are cancelled when infrastructure fails, and nurses trained at public expense work in coffee shops while the wards are short-staffed
Next: England's second-largest police force may have failed to record as many as 46,000 incidents of force used by its own officers. The technology deployed to compensate has false positive rates the forces cannot explain and error distributions they have not audited.




